Smoking crack cocaine is one of the quickest ways to develop a dangerous health condition called crack lung. While any form of cocaine is hazardous to physical and mental health, smoking crack cocaine is highly addictive, with a higher risk of long-term lung disease and pulmonary complications than snorting cocaine. Many people wonder what does crack do to your lungs, and the answer lies in its ability to cause severe inflammation and permanent tissue damage within a short period of time.
There is a direct relationship between cocaine use and crack cocaine addiction in the United States. Each year roughly 5.9 million people will abuse cocaine, and 1.4 million will freebase cocaine, also known as smoking crack.
Crack lung is an acute pulmonary syndrome you’ll develop within 48 hours of smoking crack cocaine. The inhaled vapors cause direct toxic injury to your alveoli, triggering diffuse alveolar damage that leads to inflammation, hemorrhage, and edema throughout your lung tissue. You’ll experience chest pain, fever, hemoptysis, and rapidly declining oxygen levels as your respiratory function deteriorates. Understanding the full timeline, diagnostic markers, and treatment pathways can help you recognize when this condition requires urgent intervention.
Smoking Crack Cocaine
Smoking crack cocaine is a cheaper, faster way for cocaine users to get high.
Smoking crack cocaine causes an almost instant high, but the effects are short-lived, meaning users need to take frequent hits to keep the buzz going. The fast and powerful impact, combined with the repetitive use to stay high, makes crack a highly addictive illicit drug.
Crack cocaine is one of two forms of cocaine; the other is a loose white powder form. Crack cocaine is a solid, rock form that gets its name from the cracking and popping noise it makes when it heats up.
Dealers make crack by reducing or “cooking” cocaine with water and ammonia until it dissolves, leaving crystals behind, then mixing it with other substances that can bulk up the product to make it cheaper and more potent. Most of these substances, like detergent or boric acid, are toxic, especially when burned and inhaled.
Crack cocaine users use pipes, improvised pipes, or foil to inhale crack fumes. Inhaling fumes and ash from plastic, foil, and other materials puts users at a higher risk of lung damage and disease.
Crack cocaine users use pipes, improvised pipes, or foil to inhale crack fumes, and discussions about inhaled drugs often lead people to ask questions like what is sherm. Inhaling fumes and ash from plastic, foil, and other materials puts users at a higher risk of lung damage and disease.
The desired effects of smoking crack cocaine include:
- Increased alertness
- Confidence
- Feelings of euphoria
- Increased sex drive
- Decreased appetite
- Heightened sensitivity to stimuli
People who smoke crack have a higher risk of respiratory failure, cocaine-induced psychosis, pulmonary cocaine toxicity, and life-threatening, irreversible long-term effects, including crack lung.
What Is Crack Lung?
Medical professionals use the term crack lung to broadly describe the respiratory injuries and complications caused by smoking crack cocaine. For those wondering what is crack lung, it refers to a severe pulmonary condition marked by inflammation, bleeding, and scarring of the lung tissues caused by inhaling crack smoke and other toxic chemicals.
Crack lung is an acute pulmonary and lung disease resulting from smoking crack cocaine; it can develop after prolonged use or as quickly as 48 hours after heavy crack smoking. The pulmonary system includes the airways, heart, lungs, arteries, veins, and blood vessels.
One of the most famous possible cases of crack lung was singer Amy Winehouse, who in 2008 announced she was suffering from “early signs of emphysema” and was seeking treatment. Previous to the announcement, footage of Winehouse smoking what appeared to be crack leaked to the press, leading to speculation that her health condition was pulmonary complications from drugs. Winehouse later died at age 27, joining the fabled 27 Club with other musicians who struggled with drug abuse.
One of the most famous possible cases of crack lung was singer Amy Winehouse, who in 2008 announced she was suffering from “early signs of emphysema” and was seeking treatment. Prior to the announcement, footage of Winehouse smoking what appeared to be crack leaked to the press, leading to speculation that her health condition involved pulmonary complications from drug use, alongside broader concerns about substances such as ghb. Winehouse later died at age 27, joining the fabled 27 Club with other musicians who struggled with drug abuse.
Crack lung has similar symptoms to emphysema or pneumonia, including shortness of breath, chest pain, and coughing. What starts as inflamed and irritated lung tissue, crack lung can quickly progress into respiratory failure and possibly death. However, pneumonia will heal with proper treatment, and emphysema is extremely rare in people under 40.
Once lung tissue scars, doctors consider it irreparably damaged and stress that there is a small window of time to treat crack lung properly to avoid permanent damage and death.
Possible pulmonary complications from crack lung include:
- Fluid in the lungs
- Blood in the lungs
- Blocked arteries
- Scarred lung tissue
- Damaged esophagus and trachea
- Weakened immune system
- Higher risk of tuberculosis
- Worsened asthma
- Air escaping the lungs into the chest cavity
- Lung tissue death
- Collapsed lung
- Respiratory failure
- Coma
- Death
Doctors who’ve examined patients with crack lung symptoms report the lungs sound crackly, like someone crumpling up cellophane. In many diagnostic cases, a crack lung CT scan helps reveal how much damage has occurred and whether there are visible ground-glass opacities or scarring within the lungs.
To diagnose crack lung, CT scans and chest X-rays (CXR) are the fastest course of action for emergency departments, especially when the person is not honest about drug abuse. Crack lung CT scan and crack lung radiology images and crack lung CXR will show ground glass opacities (GGO), which appear like shattered or spun glass inside the lungs. GGOs show inflammation, fluid, puss, or scar tissue and help medical professionals figure out how severe the issue is and the best course of treatment.
Crack Lung Symptoms You Shouldn’t Ignore
If you’ve smoked crack cocaine and experience chest pain with fever, you’re showing warning signs that demand immediate medical attention. Coughing up blood or producing dark, carbonaceous sputum indicates potential alveolar hemorrhage or thermal injury to your respiratory tract. When you notice rapid, shallow breathing or can’t catch your breath, your oxygen levels may have dropped dangerously low, signaling acute pulmonary compromise.
Chest Pain and Fever
When you smoke crack cocaine, your lungs can mount a severe inflammatory response within 48 hours, producing two warning signs you shouldn’t dismiss: chest pain and fever.
Chest pain develops as crack cocaine triggers diffuse alveolar injury and hemorrhagic alveolitis. Your pulmonary capillaries become increasingly permeable, leading to non-cardiogenic pulmonary edema that compromises oxygen exchange. This damage can progress to respiratory failure if you don’t seek immediate medical attention.
Fever typically registers around 38°C and signals your body’s inflammatory cascade in response to thermal airway injury and direct cellular toxicity. You’ll likely experience concurrent tachypnea and hypoxia, with oxygen saturation potentially dropping to 60-86% on room air.
These symptoms demand urgent evaluation, as acute myocardial ischemia must be ruled out in anyone presenting with crack-related chest pain.
Coughing Up Blood
How quickly can crack cocaine turn your lungs into a bleeding battlefield? Within 48 hours of smoking crack, you may experience hemoptysis, coughing up blood that signals serious crack cocaine lung damage. This occurs when thermal injury and vasospasm rupture your delicate alveoli, causing hemorrhagic alveolitis.
| Diagnostic Finding | Clinical Indicator | Severity Marker |
|---|---|---|
| Ground-glass opacities | Diffuse alveolar infiltrates | Respiratory failure risk |
| Hemosiderin-laden macrophages | Carbonaceous debris in lavage | Active bleeding confirmed |
| Bronchial wall thickening | Crazy paving pattern on CT | Chronic damage present |
You’ll notice blood-tinged sputum accompanying severe dyspnea and hypoxia. Your oxygen saturation may plummet to 80% on room air. Don’t ignore these warning signs, they indicate life-threatening pulmonary hemorrhage requiring immediate medical intervention with oxygen support and potential bronchoscopy.
Breathing Difficulty Signs
Because crack cocaine‘s toxic byproducts assault your respiratory system rapidly, you’ll experience dyspnea within 48 hours of smoking, a warning sign that acute pulmonary syndrome has begun damaging your lung tissue.
Your labored breathing develops as inflammation compromises alveolar function, reducing oxygen transfer to your bloodstream. You’ll notice breathing becomes increasingly difficult, and without intervention, respiratory failure becomes a genuine risk. These crack lung symptoms demand immediate attention.
Black phlegm accompanies your shortness of breath in approximately 65% of cases, indicating severe pulmonary irritation. Poor blood flow caused by lung inflammation creates oxygen deprivation throughout your body.
You shouldn’t dismiss these respiratory distress signals. Your lungs are communicating acute damage that requires medical evaluation before chronic complications develop.
How Fast Does Crack Lung Develop After Smoking?
Crack lung typically develops within 48 hours of smoking freebase cocaine, making it an acute pulmonary syndrome that demands rapid clinical recognition. The smoking crack effects trigger immediate inflammatory responses in your alveoli, causing direct cellular toxicity and vasospasm that rapidly compromise respiratory function.
You’ll experience dyspnea, hemoptysis, and hypoxemia as pulmonary complications cocaine use induces progress. Chest imaging reveals ground-glass opacities and diffuse infiltrates within this critical 48-hour window. The pathophysiology involves thermal injury, barotrauma, and hemorrhagic alveolitis from inhaled contaminants.
During crack cocaine overdose scenarios involving binge use, your symptoms intensify quickly. However, if you discontinue use promptly, infiltrates and respiratory distress often resolve within 36 hours. This rapid reversibility underscores why early intervention prevents permanent alveolar damage and respiratory failure.
Life-Threatening Complications of Crack Lung
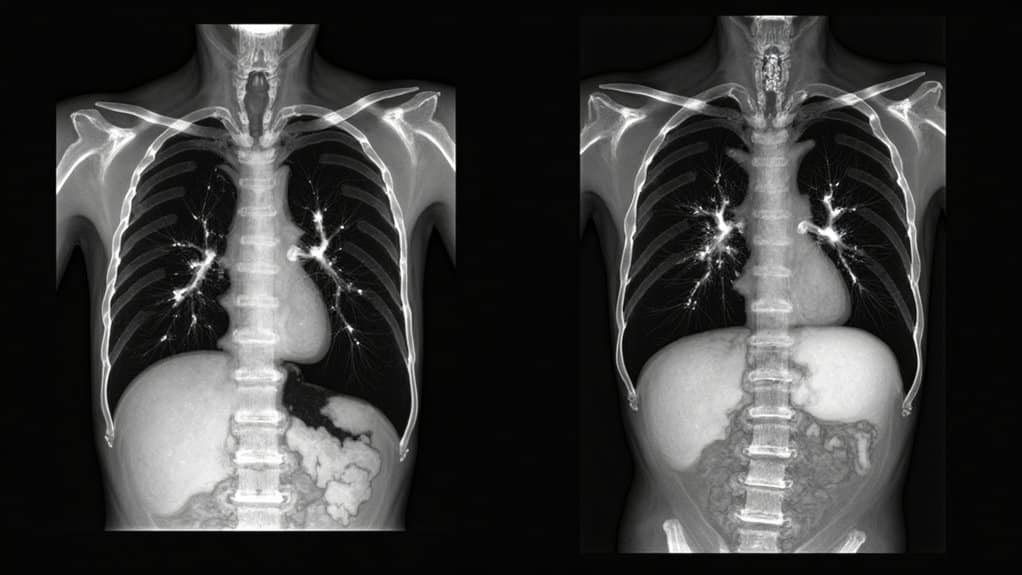
When crack lung progresses beyond its initial 48-hour window without intervention, you’re facing life-threatening complications that can rapidly prove fatal. Emergency medicine protocols prioritize identifying respiratory failure, characterized by hypoxemia with diffuse alveolar infiltrates and fever.
| Complication | Pathophysiology | Clinical Presentation |
|---|---|---|
| Respiratory Failure | Prolonged inflammatory pulmonary injury | Dyspnea, rapid infiltrates, hypoxemia |
| Pulmonary Hemorrhage | Alveolar damage with vessel constriction | Hemoptysis, bilateral opacities |
| Cardiovascular Strain | Heightened heart rate, vasoconstriction | Heart attack, stroke, arrhythmia |
| Pneumothorax | Alveolar rupture from deep inhalation | Unilateral chest pain, dyspnea |
| Noncardiogenic Edema | Fluid accumulation without cardiac involvement | Perihilar opacification |
You’ll notice hemorrhagic complications manifest as hemoptysis with multifocal bilateral opacities on radiographs. Cardiovascular strain compounds respiratory distress through vessel constriction, interrupting blood flow and triggering cardiac events even in previously healthy individuals.
How Doctors Diagnose Crack Lung
When you arrive at the hospital with respiratory symptoms after smoking crack cocaine, your doctor will rely on a combination of clinical history and imaging studies to reach a diagnosis. You’ll need to provide an accurate account of your drug use within the past 48 hours, as this temporal relationship between crack inhalation and symptom onset serves as the primary diagnostic criterion. Your physician will order chest CT imaging, which typically reveals diffuse ground-glass opacities with a characteristic “crazy-paving” pattern, often concentrated in the upper lobes and perihilar regions.
Imaging Tests Used
How do clinicians confirm crack lung when a patient presents with acute respiratory distress after smoking cocaine? Your doctor will order a chest X-ray first, which typically reveals diffuse bilateral alveolar infiltrates and focal consolidations. These findings often regress within days after you stop using.
If X-ray results appear nonspecific, you’ll undergo a CT chest scan. This imaging shows diffuse ground-glass opacities bilaterally, often sparing the periphery, with patchy air bronchograms. According to NIDA research, these patterns can mimic COVID-19 or pulmonary embolism.
Your physician may order CT angiography to exclude vascular complications. When diagnosis remains unclear, bronchoalveolar lavage helps rule out infection and hemorrhage while detecting carbonaceous debris and hemosiderin-laden macrophages. These findings, correlated with your cocaine use history, confirm the diagnosis.
Clinical History Assessment
Because crack lung lacks pathognomonic findings, your physician relies heavily on clinical history to establish the diagnosis. When you present with acute respiratory distress, your doctor will conduct a thorough inquiry focusing on recent substance use.
Key historical elements your physician assesses include:
- Temporal relationship: Symptoms typically manifest within 48 hours of crack cocaine inhalation
- Route confirmation: Direct questioning about smoking as the administration method
- Usage pattern: Frequency and duration of crack cocaine use over time
- Polysubstance assessment: Concurrent cannabis or other drug consumption
Your doctor correlates this history with presenting symptoms, dyspnea, hemoptysis, chest pain, and non-productive cough. Urine toxicology confirms cocaine exposure. Rapid symptom resolution following discontinuation strongly supports the diagnosis, distinguishing crack lung from infectious or cardiogenic etiologies.
What Crack Lung Looks Like on Imaging
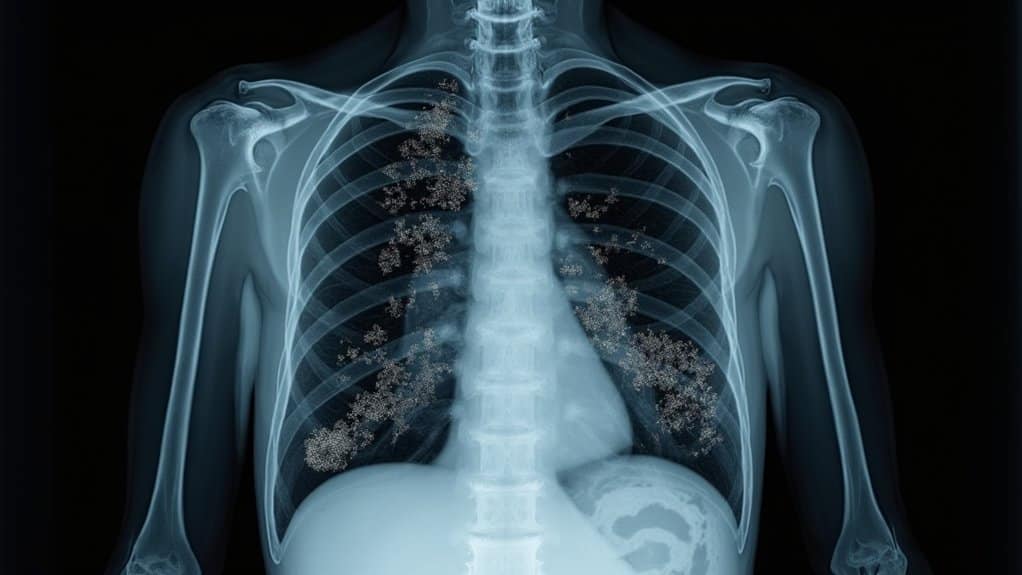
Imaging plays a critical role in diagnosing crack lung, as radiographic findings often reveal characteristic patterns that distinguish this condition from other pulmonary pathologies. On chest X-ray, you’ll typically observe bilateral perihilar opacities without cardiomegaly or pleural effusion. Ground-glass opacities frequently appear in the lower lobes, suggesting edema, hemorrhage, or aspiration.
CT imaging provides greater diagnostic specificity. You’ll notice multifocal ground-glass attenuation with interlobular septal thickening, chiefly affecting the upper lobes in a perihilar distribution. Air bronchograms and centrilobular nodules may indicate pulmonary hemorrhage. These findings can mimic COVID-19 pneumonia, requiring careful clinical correlation.
A hallmark feature distinguishing crack lung from other conditions is rapid radiographic resolution, often within hours to days after drug cessation. This transient nature helps confirm your diagnosis when clinical history correlates appropriately.
Can Your Lungs Heal After Crack Lung?
Whether your lungs can recover from crack lung depends largely on how quickly you stop using the drug and the extent of tissue damage you’ve sustained.
Clinical evidence demonstrates that acute manifestations, pulmonary infiltrates, ground-glass opacities, and bronchospasm, often resolve rapidly following cocaine cessation. Your alveolar tissue possesses regenerative capacity when you eliminate the causative agent promptly.
Several factors influence your recovery trajectory:
- Drug cessation timing: Immediate discontinuation promotes faster resolution of acute inflammation
- Co-substance use: Concurrent marijuana or tobacco use delays healing and worsens inflammation
- Baseline health: Absence of pre-existing cardiopulmonary conditions supports better outcomes
- Chronicity of use: Prolonged inhalation causes interstitial fibrosis, reducing reversibility potential
Hemosiderin-laden macrophages in your lung tissue indicate prior damage but confirm your body’s repair mechanisms have activated.
Treatment Options for Crack Lung Recovery
Once you’ve stopped using crack cocaine, your body can begin healing, but you’ll likely need medical support to manage acute respiratory compromise.
Supportive Care
Your treatment team will likely administer supplemental oxygen to correct hypoxemia. High-flow nasal cannula or CPAP with helmet delivery addresses oxygenation deficits. Chest X-rays guide diagnostic decisions when you present with dyspnea or chest pain.
Oxygen therapy and advanced respiratory support help restore breathing while imaging guides your care team’s next steps.
Pharmacological Interventions
Physicians may prescribe high-dose corticosteroids, particularly methylprednisolone, which benefits severe cases. You’ll typically see improvement within 24 hours. Antibiotics like amoxicillin/clavulanate address concurrent pulmonary infections, while enoxaparin prevents thromboembolic complications.
Ventilatory Support
If respiratory failure develops, you may require non-invasive positive pressure ventilation or endotracheal intubation with mechanical ventilation.
Outcomes
With appropriate supportive measures, most patients achieve significant clinical and radiologic improvement, often discharging within three days.
Treat Crack Cocaine Addiction at Northridge Addiction Treatment Center
Crack cocaine addiction can happen to anyone, and everyone deserves a chance to live a fulfilling, healthy life. At Northridge Addiction Treatment Center, we take a holistic, whole-person approach to overcoming addiction and treating the disease, not just the symptoms.
In the privacy of our residential treatment center, we provide onsite medical detox to get you through the physical and psychological withdrawal from crack cocaine with 24-hour medical care and support.
After detox, our dedicated and licensed staff at NATC works with each resident to develop a personalized treatment plan for your unique needs and goals. Through individual therapy, group therapy, and support groups, you will build a support network and learn healthy and productive skills to help you achieve life-long recovery.
We are eager to speak with you and help you take the first steps toward recovery. Reach out to us now.
Your Journey to Sobriety Starts Now
Crack lung is a severe and potentially fatal pulmonary complication of cocaine use recognizing its signs and symptoms early can be the difference between a medical emergency and a life-saving intervention. Northridge Treatment Center provides evidence-based medically supervised detox Los Angeles built to address every aspect of addiction with clinical precision and genuine compassion. Serving individuals throughout Encino, our +1 (855) 584-3819 team is available around the clock ready to help you take the next step toward lasting recovery.
Frequently Asked Questions
How Many People in the United States Use Crack Cocaine Each Year?
You’ll find that approximately 0.3-0.8% of Americans use crack cocaine annually, depending on demographic group. Based on 2019 data, you’re looking at hundreds of thousands of users, with 63,912 seeking treatment that year alone. When you’re evaluating patients for crack lung, remember that 18-25 year-olds show the highest cocaine use rates at 5.3%. You should screen for pulmonary complications in any patient presenting with unexplained respiratory distress and substance use history.
Does Smoking Crack With Marijuana or Tobacco Make Lung Damage Worse?
Yes, smoking crack with marijuana or tobacco worsens your lung damage. When you combine these substances, you’re exposing your respiratory system to additive irritants that compound crack’s already harmful effects. You’ll face heightened risks of alveolitis, eosinophilic pneumonia, and severe airflow obstruction. Studies of heavy crack users who also smoke marijuana or tobacco show accelerated progression of acute respiratory symptoms and increased chronic complications at the alveolar-capillary level.
Can You Experience Crack Lung Symptoms More Than Once From Repeated Use?
Yes, you can experience crack lung symptoms multiple times with repeated use. Each time you inhale crack smoke, you’re triggering pulmonary vasoconstriction, endothelial damage, and inflammatory responses that injure your alveoli. Studies show crack lung occurs in up to 20% of hospitalized users, often within 48 hours of smoking. Your lungs sustain cumulative damage, scarring, hemorrhage, and chronic inflammation, that doesn’t fully heal, making each subsequent episode potentially more severe.
Why Does Smoking Crack Cocaine Cause Black Mucus or Dark Phlegm?
When you smoke crack cocaine, you inhale combustion products containing carbonaceous material small enough to reach your alveoli. These carbon pigments deposit throughout your respiratory tract, accumulating in both intracellular and extracellular spaces within your macrophages. Your body’s alveolar and bronchiolar macrophages become laden with carbon, producing the characteristic black sputum. Additionally, you may experience alveolar hemorrhage, which contributes further to the dark pigmentation you’re expectorating.
How Does Crack Cocaine Weaken the Immune System and Increase Infection Risk?
Crack cocaine directly interferes with your white blood cells‘ normal function, disrupting both innate and adaptive immune responses. It binds to dopamine receptors on your T lymphocytes, B lymphocytes, and natural killer cells, impairing their ability to fight pathogens. You’ll also experience heightened pro-inflammatory cytokines like IL-6 and TNFα while anti-inflammatory IL-10 decreases. This inflammatory imbalance, combined with direct lung tissue damage, substantially increases your susceptibility to pneumonia, bronchitis, and other respiratory infections.




